Inflammatory Pain
Updated:
What is inflammatory pain?
Inflammatory pain is a generic term given to pain that occurs in association with an inflammatory response and typically last 48 – 72 hours following injury or injury aggravation.
Part of the inflammatory response is the accumulation of swelling and chemicals that cause pain in the injured tissue. The accumulation of these chemicals occurs in any position and often in greater quantities with inactivity. This results in symptoms that are present regardless of position and often may increase with rest (such as at night or upon waking in the morning) especially following aggravating activity. Inflammatory symptoms are often described as constant, dull, aching or, in some cases, throbbing.
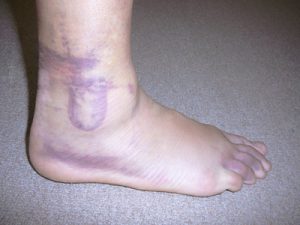
Inflammatory vs. Mechanical Pain
The pain associated with a typical musculoskeletal injury can generally be categorised as being inflammatory, mechanical, or having co-existing mechanical and inflammatory elements.
Whilst inflammatory pain is often constant, mechanical pain tends to come and go and is typically dependent upon position. Patients with mechanical pain experience symptoms that can be relieved or provoked with certain activities or positions that place specific forces on injured tissue. These provocative activities are often reproducible, with patients’ typically experiencing cessation of symptoms when these forces are removed.
In injuries with typical inflammatory symptoms, pain is not alleviated with a change in position, but instead may decrease in severity with general movement, heat treatment (such as taking a hot shower or using a hot pack), massage or alcohol consumption. It is important to note however, that although a reduction in symptoms may be obtained with general movement, heat, massage or alcohol, these modalities will actually increase total inflammation (after these activities with rest).
Causes of inflammatory pain
Inflammatory pain frequently occurs in the first 48 – 72 hours following injury or injury aggravation. Injury (or injury aggravation) occurs when stress on the affected tissue is greater than it can withstand, often due to repetitive, prolonged or traumatic forces.
Traumatic forces that may be responsible for sudden onset injuries and subsequent inflammatory pain may include:
- heavy lifting
- a fall or collision
- an awkward landing
- sudden take off
- twisting incident
- motor vehicle accident
In injuries with a more gradual onset, repetitive or prolonged forces (often with inadequate recovery periods) are frequently to blame such as excessive weight bearing activity (e.g. too much standing, walking or running), overuse of a specific body part, excessive work, sport, housework or recreational activity participation, excessive use of devices (such as computers, or mobile phones), or poor postural positions such as excessive sitting (e.g. whilst driving, at a computer or when watching television).
Most injuries have the capacity to produce inflammatory pain. Some of the most common causes of inflammatory pain include:
- Joint injuries (such as sprains or dislocations)
- Ligament tears
- Cartilage injuries (such as tears or degeneration)
- Nerve injuries (such as a pinched nerve)
- Arthritis
- Intervertebral disc injuries
- Bone injuries (such as fractures, stress fractures or contusions)
- Other soft tissue inflammation such as bursitis or synovitis
Signs and symptoms of inflammatory pain
Inflammatory pain is often described as constant, dull, aching or, in some cases, throbbing. Patients with inflammatory pain typically experience pain or ache that increases with rest (often at night or upon waking in the morning) especially following aggravating activity.
Symptoms may temporarily decrease with heat, massage, alcohol consumption and general movement or exercise (all of which increase blood flow to the local region and subsequently temporarily transport chemicals away from the local tissue). This increased blood flow however is responsible for the transportation of more inflammatory cells resulting in even greater inflammation during the subsequent rest period.
Patients with inflammatory pain may experience an increase in pain with a change in position, however, pain typically can not be completely alleviated in this manner. Tenderness is usually experienced upon firmly touching the affected tissue. A broader region of diffuse tenderness is also often experienced due to the accumulation of inflammatory chemicals and swelling. Observable swelling, colour change of local tissue (such as redness) and an increase in local tissue temperature are other common symptoms that may be experienced in association with inflammation.
Other symptoms can vary considerably depending on the nature and severity of the injury and may include:
- A feeling of weakness
- Clicking, grinding, locking or catching sensations
- Giving way of a particular body part
- A limp (for lower limb injuries)
- Restricted joint mobility or flexibility
- Pins and needles or numbness
Diagnosis of inflammatory pain
A thorough examination from a physiotherapist is usually sufficient to diagnose the presence of inflammatory pain and the underlying cause. Investigations such as X-ray, ultrasound, CT scan and MRI are sometimes used to confirm diagnosis and exclude the presence of other injuries.
General treatment principles for inflammatory pain

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Surgery for inflammatory pain
A small percentage of patients who experience inflammatory pain (due to specific conditions) may require surgery to ensure an optimal outcome. Others may also require surgical intervention if their condition has not responded adequately to an appropriate physiotherapy program. Some common causes of inflammatory pain requiring surgical intervention include:
- Certain fractures (requiring realignment, internal fixation or bone grafting)
- Severe osteoarthritis (requiring joint replacement surgery)
- Severe cartilage injuries (requiring arthroscopic debridement)
- Full thickness muscle, tendon or ligament tears (requiring surgical repair)
- Joint dislocation (requiring stabilisation surgery)
- Severe spinal conditions often with associated arm or leg pain (requiring procedures such as discectomy, laminectomy or spinal fusion)
Prognosis for inflammatory pain
The prognosis of inflammatory pain is largely dictated by the severity of the injury and the specific tissue affected. Most inflammatory pain has the capacity to subside within 48 – 72 hours, however the underlying condition may take longer to completely resolve. In minor injuries a full recovery may take place within days to weeks, whilst more severe cases (particularly those involving surgery) may take many months or sometimes years and may sometimes require other intervention or procedures to ensure an optimal outcome.
Contributing factors to the development of inflammatory pain
There are several factors which may predispose patients to developing inflammatory pain. These can vary based on the specific injury and tissue affected. A physiotherapist can usually identify these factors and correct them as part of appropriate treatment. Some of them may include:
- excessive or inappropriate training or activity
- inadequate rest or recovery periods from training or activity
- a lifestyle involving repetitive, prolonged or heavy forces
- inadequate rehabilitation for a previous injury
- sub-optimal biomechanics
- poor posture
- poor sporting technique
- muscle tightness or weakness
- joint stiffness
- inadequate warm up
- inadequate fitness
- fatigue
- poor core or pelvic stability
- poor control or balance
- genetic predisposition
- deconditioning
- obesity or being overweight
Physiotherapy for inflammatory pain
Physiotherapy treatment is vital to hasten the healing process and ensure an optimal outcome in patients with inflammatory pain due to a musculoskeletal injury (regardless of whether they require other intervention). Treatment will vary based on the condition causing the inflammatory pain and stage of healing and rehabilitation. Physiotherapy treatment may comprise:
- soft tissue massage (once inflammation has settled or immediately to adjacent areas)
- joint mobilization
- joint manipulation
- electrotherapy
- taping or bracing
- the use of other supportive devices such as crutches, walking sticks, protective boots, slings etc.
- dry needling
- hydrotherapy
- ice or heat treatment
- the use of compression bandages
- elevation of the affected body part
- anti-inflammatory advice
- progressive exercises to improve flexibility, balance, strength, control, cardiovascular fitness and function
- activity modification advice
- biomechanical and postural correction
- education
- weight loss advice where appropriate
- a gradual return to sport or activity program
Other intervention for inflammatory pain
Despite appropriate physiotherapy management, some patients with inflammatory pain fail to improve adequately either conservatively or following surgery. When this occurs the treating physiotherapist or doctor can advise on the best course of management. This may include further investigations, pharmaceutical intervention, injection therapy (e.g. cortisone, pain relieving or blood injection), minimally invasive procedures or surgery.
Exercises for inflammatory pain
Patients with inflammatory pain frequently benefit from progressive, pain free exercises to improve flexibility, strength, function and control of the injured area depending on the specific injury and stage of healing. There should also be no increase in symptoms after the exercises with rest (e.g. that night or upon waking the following morning). You should discuss the suitability of any exercises with your physiotherapist prior to beginning them. Below is a list of flexibility and strengthening exercises commonly used in rehabilitation for various injuries:
Joint Strengthening Exercises
- Ankle Strengthening
- Elbow Strengthening
- Hand Strengthening
- Hip Strengthening
- Knee Strengthening
- Lower Back Strengthening
- Neck Strengthening
- Shoulder Strengthening
- Upper Back Strengthening
- Wrist Strengthening
Joint Stretches
- Ankle Stretches
- Elbow Stretches
- Hand Stretches
- Hip Stretches
- Knee Stretches
- Lower Back Stretches
- Neck Stretches
- Shoulder Stretches
- Upper Back Stretches
- Wrist Stretches
Other Common Rehabilitation Exercises
 Physiotherapy products for inflammatory pain
Physiotherapy products for inflammatory pain
Some of the most commonly recommended products by physiotherapists to hasten healing and speed recovery in patients with inflammatory pain include:
To purchase physiotherapy products for inflammatory pain click on one of the above links or visit the PhysioAdvisor Shop.
 Find a Physio to assist with inflammatory pain
Find a Physio to assist with inflammatory pain
Find a physiotherapist in your local area who can identify and treat the underlying cause of inflammatory pain.
 More Information
More Information
- R.I.C.E Regime
- Ice or Heat
- Mechanical Pain
- Injuries
- Posture
- Mobile Phone Ergonomics
- Ergonomic Computer Setup
- Safe Lifting
- Choosing a School Bag
- Choosing a Shoe
- Do I Need Orthotics
- Injury Prevention
- Sports Recovery
- Warm Up & Cool Down
- How to Use Crutches
- Investigations
- Returning to Running
- Return to Sport
- Bike Setup
- Understanding Pain
 Physiotherapy Exercises
Physiotherapy Exercises
- View our large range of Physiotherapy Exercises
Become a PhysioAdvisor Member
-
 Individual Membership (12 Months)$59.95 for 1 year
Individual Membership (12 Months)$59.95 for 1 year -
 Individual Membership (3 Months)$39.95 for 3 months
Individual Membership (3 Months)$39.95 for 3 months -
 Individual Membership (Yearly)$49.95 / year
Individual Membership (Yearly)$49.95 / year -
 Individual Membership (Monthly)$15.95 / month
Individual Membership (Monthly)$15.95 / month

Link to this Page
If you would like to link to this article on your website, simply copy the code below and add it to your page:
<a href="https://physioadvisor.com.au/health/injury-rehabilitation/inflammatory-pain-inflammation”>Inflammatory Pain – PhysioAdvisor.com</a><br/>Detailed physiotherapy information on Inflammatory Pain including key treatment principles written by PhysioAdvisor's experienced physiotherapists.
Return to the top of Inflammatory Pain.