Knee Arthritis (Osteoarthritis)
Updated:
(Also known as Knee Osteoarthritis, Osteoarthritis of the Knee, Arthritis of the Knee, Degeneration of the Knee)
N.B. The term ‘knee arthritis’ will be used in this document to describe the condition known as knee osteoarthritis.
What is knee arthritis?
Knee arthritis is a condition characterized by a degenerative process whereby there is gradual wear and tear to the cartilage and bone surfaces of the knee joint with subsequent inflammation. Knee arthritis may occur following a specific injury or due to repetitive forces going through the knee joint beyond what it can withstand over a period of time.
In a normal knee, joint surfaces are smooth and there is cartilage between the bone ends which allows for efficient shock absorption and smooth movement (figure 1).
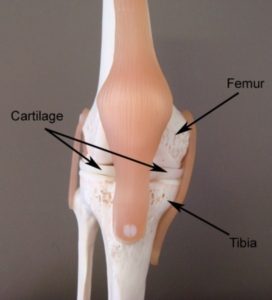
When the knee is damaged or overloaded, particularly with excessive weight-bearing or twisting forces, degeneration of the cartilage can occur, reducing the knee’s shock absorbing capacity. As the condition progresses, and the cartilage wears away, the joint space can narrow and there is eventual wearing down of the bone ends so that the surfaces are no longer smooth (figure 2). The bone ends may also develop small bony processes (spurs) called ‘osteophytes’. When some or all of these changes occur, the condition is known as knee arthritis.
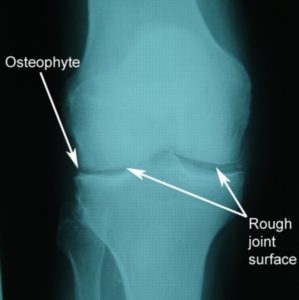
Arthritis of the knee usually occurs after the age of 50 years and tends to affect females more frequently than males. It is more common in those patients who are overweight or have a past history of injury, surgery or trauma to the knee.
Signs and symptoms of knee arthritis
Patients with this condition usually experience symptoms that develop gradually over time. In patients with minor cases of knee arthritis, little or no symptoms may be present. As the condition progresses, there may be increasing knee pain with weight bearing activity and joint stiffness (particularly after rest or first thing in the morning). Swelling, decreased flexibility (i.e. an inability to fully straighten or bend the knee), severe joint pain, pain at night and a grinding, clicking or locking sensation during certain movements may also be experienced. Symptoms can sometimes fluctuate from month to month with patients reporting an increase in symptoms with colder weather. In more severe cases, muscle wasting (especially of the quadriceps), a visible deformity of the knee joint, and a limp may also be present.
Diagnosis of knee arthritis
A thorough subjective and objective examination from a physiotherapist may be sufficient to diagnose knee arthritis. An X-ray is usually required to confirm diagnosis and may demonstrate signs of decreased joint space, irregularities of the bony ends and/or the presence of bony spurs (osteophytes). Sometimes an MRI may also be indicated to assist with diagnosis and rule out other pathologies.
Treatment for knee arthritis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Prognosis of knee arthritis
Because knee arthritis is a progressive condition, complete resolution of symptoms is often not possible. However, in mild to moderate cases, most patients, if managed well, can maintain an active lifestyle with little or no symptoms and delay or prevent the deterioration of the condition. In severe cases that have been unresponsive to appropriate physiotherapy management and where quality of life is significantly affected, knee joint replacement surgery is usually indicated with most patients subsequently experiencing a good outcome following the procedure.
Physiotherapy for knee arthritis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Contributing factors to the development of knee arthritis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Other intervention for knee arthritis
Despite appropriate physiotherapy management, some patients with arthritis of the knee continue to deteriorate. When this occurs, other intervention may be required. This may include pharmaceutical intervention, corticosteroid injection, the use of supplements such as fish oil, glucosamine and chondroitin, investigations such as an X-ray, CT scan, bone scan or MRI, or assessment from a specialist.
In more advanced cases of knee arthritis, where symptoms are severe and quality of life severely affected, patients may require surgical intervention. This may involve a knee arthroscope or partial or complete knee joint replacement surgery. The treating physiotherapist or doctor can advise if this may be required and will refer to an orthopaedic specialist for an assessment and opinion.
Following a total knee joint replacement, patients are normally in hospital for 5 to 10 days afterwards and require physiotherapy treatment and rehabilitation over the following months. Resumption of normal daily activity can usually be achieved 6 – 12 months following surgery.
Exercises for knee arthritis
The following exercises are commonly prescribed to patients with arthritis of the knee. You should discuss the suitability of these exercises with your physiotherapist prior to beginning them. Generally, they should be performed 3 times daily once the physiotherapist has indicated it is safe to do so and only provided they do not cause or increase symptoms.
Your physiotherapist can advise when it is appropriate to begin the initial exercises and eventually progress to the intermediate and advanced exercises. As a general rule, addition of exercises or progression to more advanced exercises should take place provided there is no increase in symptoms.
Initial Exercises
Knee Bend to Straighten
Lying on your back, slowly bend and straighten your knee as far as you can go without pain and provided you feel no more than a mild to moderate stretch (figure 3). Repeat 10 times.
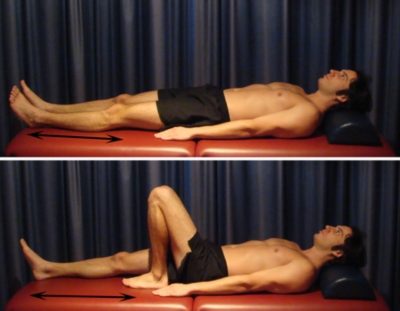
Static Quadriceps Contraction
With your knee relatively straight, slowly tighten the muscle at the front of your thigh (quadriceps) by pushing your knee down into a small rolled up towel (figure 4). Put your fingers on your quadriceps to feel the muscle tighten during the contraction. Hold for 5 seconds and repeat 10 times as firmly as possible without increasing your symptoms.
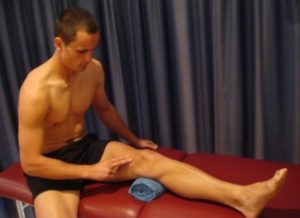
Static Hamstring Contraction
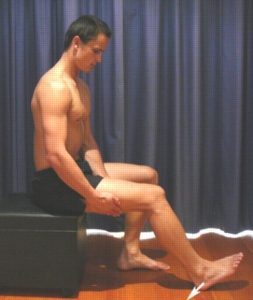
Begin this exercise in sitting with your knee bent to about 45 degrees (figure 5). Press your heel into the floor tightening the back of your thigh (hamstrings). Hold for 5 seconds and repeat 10 times as hard as possible provided the exercise is pain free.
Hip Extension in Standing
Begin this exercise standing at a table or bench for balance. Keeping your back and knee straight, slowly take your leg backwards, tightening your bottom muscles (gluteals) (figure 6). Hold for 2 seconds then slowly return to the starting position. Repeat 10 times provided the exercise is pain free.

Intermediate Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Advanced Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Other Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Rehabilitation Protocol for knee arthritis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
 Physiotherapy products for knee arthritis
Physiotherapy products for knee arthritis
Some of the most commonly recommended products by physiotherapists for patients with this condition include:
-
 Talar Made TRIO Orthotics (3/4 length)
Talar Made TRIO Orthotics (3/4 length) -
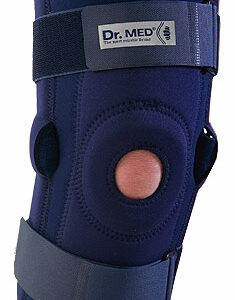 Dr Med Hinged Knee Support (Model K011)
Dr Med Hinged Knee Support (Model K011) -
 Aluminium Adjustable Walking Stick
Aluminium Adjustable Walking Stick -
 Alpha 418 Rollator Mobility 4 Wheel Walker
Alpha 418 Rollator Mobility 4 Wheel Walker -
 Forearm Crutches Adjustable – Standard Grip
Forearm Crutches Adjustable – Standard Grip -
 Fitness Ball Pro – Loumet
Fitness Ball Pro – Loumet -
 AllCare Tubing
AllCare Tubing -
 AllCare Instant Cold Pack (15 x 25cm)
AllCare Instant Cold Pack (15 x 25cm) -
 AllCare Foam Roller Round
AllCare Foam Roller Round
To purchase physiotherapy products for knee arthritis, click on one of the above links or visit the PhysioAdvisor Shop.
 Find a Physio
Find a Physio
Find a physiotherapist in your local area who can treat this condition.
 More Exercises
More Exercises
- Knee Stretches
- Knee Strengthening Exercises
- Leg Strengthening Exercises
- Leg Stretches
- Balance Exercises
- Cardiovascular Exercise
- Pilates Exercises
 Recommended Reading
Recommended Reading
- Ice or Heat
- The R.I.C.E. Regime
- Choosing a Shoe
- Do I Need Orthotics
- How to use Crutches
- Knee Taping
- Patella Taping
- Understanding Pain
- Inflammatory Pain
- Mechanical Pain
- Why is my injury not Improving?
- Knee Diagnosis Guide
Become a PhysioAdvisor Member
-
 Individual Membership (12 Months)$59.95 for 1 year
Individual Membership (12 Months)$59.95 for 1 year -
 Individual Membership (3 Months)$39.95 for 3 months
Individual Membership (3 Months)$39.95 for 3 months -
 Individual Membership (Yearly)$49.95 / year
Individual Membership (Yearly)$49.95 / year -
 Individual Membership (Monthly)$15.95 / month
Individual Membership (Monthly)$15.95 / month

Link to this Page
If you would like to link to this article on your website, simply copy the code below and add it to your page:
<a href="https://physioadvisor.com.au/injuries/knee/knee-arthritis-osteoarthritis”>Knee Arthritis (Osteoarthritis) – PhysioAdvisor.com</a><br/>We offer detailed physiotherapy information on knee arthritis (knee osteoarthritis) including causes, signs and symptoms, treatment, exercises and more.
Return to the top of Knee Arthritis (Osteoarthritis).
