Frozen Shoulder
Updated:
(Also known as Adhesive Capsulitis, Frozen Shoulder Syndrome)
What is a frozen shoulder?
A frozen shoulder is a condition characterized by inflammation, scarring and tightening of the connective tissue surrounding the shoulder joint, usually resulting in shoulder pain and a marked loss of shoulder movement.
The shoulder joint is a ball and socket joint. The shoulder blade gives rise to the socket of the shoulder, whilst the ball arises from the top of the humerus (upper arm bone). Surrounding the ball and socket joint is strong connective tissue holding the bones together known as the shoulder joint capsule (figure 1).
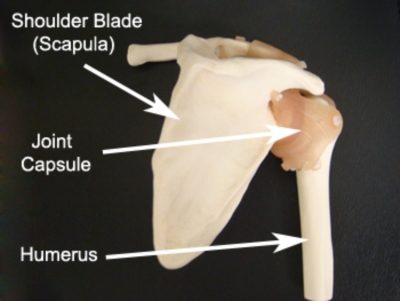
Occasionally, the shoulder joint capsule may become inflamed with subsequent tightening and scarring of the shoulder joint capsule. When this occurs the condition is known as a frozen shoulder and usually results in a marked loss of shoulder range of movement.
Frozen shoulders most commonly occur in people over 40 years of age and typically affect women more commonly than men. They can generally be divided into 3 phases, each of which can last a number of months:
- Pain – In this first phase of a frozen shoulder, the shoulder typically becomes painful with most movements. The shoulder may also start to stiffen during this phase.
- Freezing – This second phase of this condition is characterized by a marked loss of movement of the shoulder, coinciding with scarring of the shoulder joint capsule. Patients typically experience difficulty when elevating the arm or taking their hand behind their back. Pain may decrease noticeably during this phase.
- Thawing – In this final phase, the shoulder spontaneously begins to ‘loosen’ up and movement to the shoulder is gradually restored.
Causes of a frozen shoulder
Whilst the exact cause of a frozen shoulder is not exactly known, it is thought to occur following injury or damage to the shoulder joint or adjacent soft tissue. In these cases, a frozen shoulder is more likely to develop if the initial injury is not treated appropriately. This often occurs due to inadequate rest from aggravating activities or adopting a ‘no pain no gain’ attitude. A patient may also have an increased likelihood of developing the condition following excessive immobility (i.e. not moving the shoulder, particularly after injury or surgery) or if they suffer from other auto-immune diseases or diabetes.
Signs and symptoms of a frozen shoulder
The symptoms associated with this condition usually develop gradually over time (often following a recent history of shoulder injury, surgery and/or immobilisation). Patients typically experience a dull ache that may increase to a sharper pain with certain movements or activities. Pain tends to be focused deep in the shoulder, however may occasionally be experienced in the upper arm, upper back and neck. Patients may also experience stiffness in each of these regions.
The pain associated with a frozen shoulder may increase with any movement of the shoulder and with activities placing stress on the shoulder joint. These activities may include: arm elevation, lifting, carrying, pushing or pulling, lying on the affected side and taking your hand behind your back (e.g. putting on a bra). Patients with a frozen shoulder often experience pain at night or upon waking in the morning. As the condition progresses from the painful phase to the frozen phase, pain may reduce significantly.
Aside from pain, patients also typically experience marked stiffness and significantly reduced range of movement of the shoulder. This typically affects all shoulder movements, but is most noticeable with rotation and elevation. This may present as difficulty elevating the affected arm or an inability to take the hand behind the back. As this condition progresses from the frozen phase to the thawing phase, range of movement gradually increases with a subsequent reduction in joint stiffness. Patients may also develop muscle wasting in the affected arm, as the condition progresses, through lack of use.
Although a frozen shoulder generally affects only one side, some patients may develop the condition in both shoulders.
Diagnosis of a frozen shoulder
A thorough subjective and objective examination from a physiotherapist is usually sufficient to diagnose a frozen shoulder. Further investigations such as an Ultrasound or MRI scan may be required to assist diagnosis.
Treatment for a frozen shoulder

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Prognosis of a frozen shoulder
Most cases of frozen shoulder tend to settle after a number of months. In severe cases, symptoms may be present for 18 months or longer. Usually the painful stage of a frozen shoulder lasts 2 – 6 months. The frozen phase approximately 4 -12 months, whilst the thawing phase may last an additional 4 – 18 months.
In some cases, patients may experience ongoing and permanent restriction in movement following completion of all three stages. However, most cases of frozen shoulder will have a good outcome.
Contributing factors to the development of a frozen shoulder
There are several factors which can predispose patients to developing a frozen shoulder. These need to be assessed and where possible, corrected with direction from a physiotherapist. Some of these factors may include:
- a history of recent shoulder injury
- a history of recent shoulder surgery
- inappropriate treatment following shoulder injury or surgery (particularly inadequate or excessive rest)
- diabetes
- auto-immune disease
- age > 40 years
- poor posture
Physiotherapy for a frozen shoulder
Physiotherapy treatment for a frozen shoulder is vital to hasten the healing process and ensure an optimal outcome. Treatment may comprise:
- soft tissue massage
- electrotherapy (e.g. ultrasound, TENS)
- joint mobilization
- dry needling
- ice or heat treatment
- exercises to improve flexibility, strength and posture
- hydrotherapy
- education
- activity modification advice
- postural correction
- anti-inflammatory advice
- devising and monitoring an appropriate return to activity plan
Other intervention for a frozen shoulder
Despite appropriate physiotherapy management, some patients with this condition do not improve adequately or require other intervention to ensure an optimal outcome. When this occurs the treating physiotherapist or doctor can advise on the best course of management. This may include further investigations such as X-rays, ultrasound, CT scan or MRI, pharmaceutical intervention, corticosteroid injection, hydrodilatation, manipulation under anaesthetic or referral to appropriate medical authorities who can advise on any intervention that may be appropriate to improve the condition.
Exercises for a frozen shoulder
The following exercises are commonly prescribed to patients with this condition. You should discuss the suitability of these exercises with your physiotherapist prior to beginning them. Generally, they should be performed 3 times daily and only provided they do not cause or increase symptoms.
Your physiotherapist can advise when it is appropriate to begin the initial exercises and eventually progress to the intermediate, advanced and other exercises. As a general rule, addition of exercises or progression to more advanced exercises should take place provided there is no increase in symptoms.
Initial Exercises
Shoulder Blade Squeezes
Begin this exercise by standing or sitting with your back and neck straight. Your chin should be tucked in slightly (with your face looking straight ahead) and your shoulders should be back slightly. Slowly squeeze your shoulder blades together as hard and far as possible provided it does not cause or increase symptoms (figure 2). Hold for 5 seconds and repeat 10 times provided the exercise is pain free.
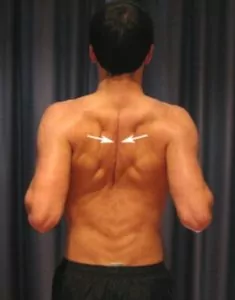
Pendular Exercises
Begin this exercise by leaning forwards with your good forearm supported on a table or bench (figure 3). Keeping your back and neck straight and your shoulder relaxed, gently swing your affected arm forwards and backwards as far as you can go without pain and provided you feel no more than a mild to moderate stretch. Repeat the exercise swinging your arm side to side provided it is pain free. Repeat 10 times each provided there is no increase in symptoms.
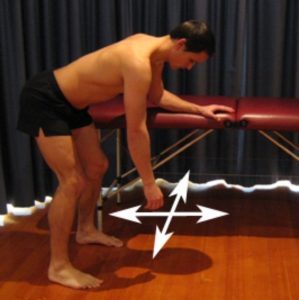
Pendular Circles
Begin this exercise by leaning forwards with your good forearm supported on a table or bench (figure 4). Keeping your back and neck straight and your shoulder relaxed, gently swing your affected arm in circles clockwise as far as you can go without pain and provided you feel no more than a mild to moderate stretch. Repeat the exercise swinging your arm counter clockwise. Repeat 10 times in each direction provided there is no increase in symptoms.
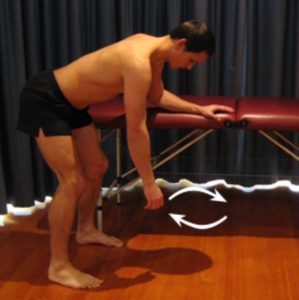
Intermediate Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Advanced Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Other Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Rehabilitation Protocol for a frozen shoulder

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
 Physiotherapy products for a frozen shoulder
Physiotherapy products for a frozen shoulder
Some of the most commonly recommended products by physiotherapists for patients with this condition include:
To purchase physiotherapy products for a frozen shoulder click on one of the above links or visit the PhysioAdvisor Shop.
 Find a Physio
Find a Physio
Find a physiotherapist in your local area who can treat a frozen shoulder.
 Other Exercises
Other Exercises
- View more Shoulder Stretches
- View more Shoulder Strengthening Exercises
- View Arm Stretches
- View Arm Strengthening Exercises
- View Upper Body Foam Roller Exercises
- View Upper Body Massage Ball Exercises
- View Upper Body Resistance Band Exercises
 More information
More information
- View detailed information on when to use Ice or Heat
- View detailed information on initial injury management and the R.I.C.E. Regime.
- View detailed information on Warming Up & Cooling Down.
- View detailed information on Returning to Sport.
- Read our Shoulder Diagnosis Guide.
Become a PhysioAdvisor Member

Link to this Page
If you would like to link to this article on your website, simply copy the code below and add it to your page:
<a href="https://physioadvisor.com.au/injuries/shoulder/frozen-shoulder”>Frozen Shoulder – PhysioAdvisor.com</a><br/>A frozen shoulder is a condition characterised by inflammation, scarring and tightening of the connective tissue surrounding the shoulder joint.
Return to the top of Frozen Shoulder.










