Calf Strain (Gastrocnemius)
Updated:
(Also known as Calf Tear, Torn Calf Muscle, Strained Calf Muscle, Pulled Calf, Gastrocnemius Strain, Gastrocnemius Tear, Torn Gastrocnemius)
What is a calf strain?
A calf strain is an injury characterized by tearing of one or more of the calf muscles and typically causes pain in the back of the lower leg.
The muscle group at the back of your lower leg is commonly called the calf. The calf comprises of 2 major muscles one of which originates from above the knee joint (gastrocnemius) the other of which originates from below the knee joint (soleus). Both of these muscles insert into the heel bone via the Achilles tendon (figure 1).
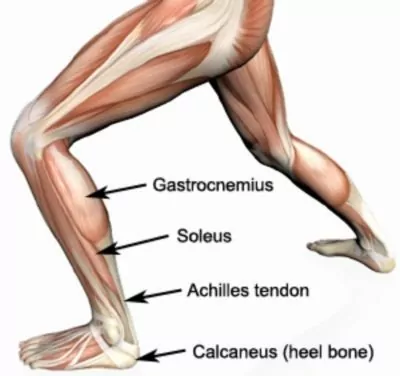
During contraction of the calf, tension is placed through the calf muscle. When this tension is excessive due to too much repetition or high force, the calf muscle can be torn. This is known as a calf strain.
Tears to the calf muscle can range from a small partial tear whereby there is minimal pain and minimal loss of function, to a complete rupture which may require surgical reconstruction.
Calf strains range from grade 1 to grade 3 and are classified as follows:
- Grade 1 Tear: a small number of fibres are torn resulting in some pain, but allowing full function.
- Grade 2 Tear: a significant number of fibres are torn with moderate loss of function.
- Grade 3 Tear: all muscle fibres are ruptured resulting in major loss of function.
The majority of calf strains are grade 2 tears and most commonly affect the gastrocnemius muscle (particularly the inner aspect i.e. medial head). Soleus strains although less common (due to the fact that the muscle only crosses one joint i.e. the ankle) are also sometimes seen in clinical practise.
Causes of a calf strain
Calf strains commonly occur due to a sudden contraction of the calf muscle (often when it is in a position of stretch). This frequently occurs when a patient attempts to accelerate from a stationary position (e.g. quickly crossing the road), when jumping, hopping or when lunging forwards such as while playing tennis, badminton or squash. Calf strains are also commonly seen in running sports such as football and athletics.
Occasionally they occur due to gradual wear and tear associated with overuse. This may be due to activities such as repetitive jumping, distance running or walking excessively (especially up hills, on uneven surfaces or whilst carrying a heavy backpack).
Signs and symptoms of a calf strain
Patients with this condition usually feel a sudden sharp pain or pulling sensation in the calf muscle at the time of injury. In minor strains, pain may be minimal allowing continued activity. In more severe cases, patients may experience severe pain, muscle spasm, weakness, and an inability to continue activity. Patients with a severe calf strain may also walk with a limp or be unable to weight bear on the affected leg.
Patients with this condition may experience pain during activities such as walking (especially uphill), going up and down stairs, running, jumping, hopping, or standing on tip toe. It is also common for patients to experience pain or stiffness after these activities with rest especially upon waking in the morning. Swelling, tenderness and bruising may also be present in the affected calf muscles. In cases of a grade 3 tear a visible and palpable deformity in the muscle may be evident.
Diagnosis of a calf strain
A thorough subjective and objective examination from a physiotherapist is usually sufficient to diagnose a calf strain. Further investigations such as an MRI scan or Ultrasound may be required, in rare cases, to confirm diagnosis and assess the severity of injury.
Treatment for a calf strain

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Prognosis of a calf strain
With appropriate management, patients with a minor calf strain can usually recover in one to three weeks. With larger tears, recovery may take four to eight weeks or longer depending on the severity. In cases of a complete rupture of the calf muscle surgery may be required with intensive rehabilitation to follow. Return to sport or activity may then take 6 months or longer.
Contributing factors to the development of a calf strain
There are several factors which can predispose patients to developing a calf strain. These need to be assessed and corrected with direction from a physiotherapist. Some of these factors include:
- poor calf flexibility
- inappropriate or excessive training or activity
- inadequate recovery periods from training or activity
- poor biomechanics or foot posture (e.g. flat feet)
- inadequate warm up
- ankle joint stiffness
- calf weakness
- inadequate rehabilitation following a previous calf strain or Achilles injury
- decreased fitness and conditioning
- fatigue
- neural tightness (sometimes in association with a lower back injury)
Physiotherapy for a calf strain
Physiotherapy for patients with a calf strain is vital to hasten the healing process, ensure an optimal outcome and minimise the likelihood of recurrence. Treatment may comprise:
- soft tissue massage
- electrotherapy (e.g. ultrasound)
- anti-inflammatory advice
- the use of heel wedges or crutches
- Achilles tendon taping
- Calf taping
- stretches
- dry needling
- joint mobilization
- ice or heat treatment
- exercises to improve strength, flexibility or balance
- hydrotherapy
- education
- activity modification advice
- biomechanical correction (e.g. the use of orthotics)
- a gradual return to activity program
- a gradual return to running program or sport
Other intervention for a calf strain
In the event of a complete rupture of the calf muscle (although rarely seen in clinical practise), surgery is sometimes indicated. It is vital that all patients with a potential calf muscle complete rupture seek physiotherapy or medical assessment as soon as possible to determine if the muscle is completely ruptured. This is vital as delayed treatment may result in a poor outcome due to shortening of the torn calf muscle. The patient’s doctor or physiotherapist may then refer on to an orthopaedic specialist if it is warranted clinically.
Surgical repair of the ruptured calf muscle is generally considered the most appropriate form of management for active individuals seeking the highest level of function. This often involves a period of immobilization in a plaster cast for one to two months following surgery and a rehabilitation period of three to six months involving extensive physiotherapy.
Conservative management of ruptured calf muscles may be appropriate, particularly for older individuals. This involves immobilising the calf in a shortened position in a cast for approximately four weeks. The calf is then gradually stretched and strengthened over time.
Exercises for a calf strain
The following exercises are commonly prescribed to patients with this condition. You should discuss the suitability of these exercises with your physiotherapist prior to beginning them. Generally, they should be performed 3 times daily and only provided they do not cause or increase symptoms.
Your physiotherapist can advise when it is appropriate to begin the initial exercises and eventually progress to the intermediate and advanced exercises. As a general rule, addition of exercises or progression to more advanced exercises should take place provided there is no increase in symptoms.
Initial Exercises
Calf Stretch with Towel
Begin this calf stretch in long sitting with your leg to be stretched in front of you. Your knee and back should be straight and a towel or rigid band placed around your foot as demonstrated (figure 2). Using your foot, ankle and the towel, bring your toes towards your head until you feel a stretch in the back of your calf, Achilles tendon or leg. Hold for 5 seconds and repeat 10 times at a mild to moderate stretch provided the exercise is pain free.

Resistance Band Calf Strengthening
Begin this exercise with a resistance band around your foot as demonstrated and your foot and ankle held up towards your head (figure 3). Slowly move your foot and ankle down against the resistance band as far as possible and comfortable without pain, tightening your calf muscle. Slowly return back to the starting position. Repeat 10 – 20 times provided the exercise is pain free.

Intermediate Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Advanced Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Other Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Rehabilitation Guide for a calf strain

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
 Find a Physio for a calf strain
Find a Physio for a calf strain
Find a physiotherapist in your local area to treat a calf strain
 Physiotherapy products for a calf strain
Physiotherapy products for a calf strain
Some of the most commonly recommended products by physiotherapists to hasten healing and speed recovery in patients with this condition include:
-
 Wheat Bags
Wheat Bags -
 Heel Lifts (Elevators – Talar Made) (Pack of 5 Pairs)
Heel Lifts (Elevators – Talar Made) (Pack of 5 Pairs) -
 Forearm Crutches Adjustable – Standard Grip
Forearm Crutches Adjustable – Standard Grip -
 AllCare Band
AllCare Band -
 Mueller Calf Wrap
Mueller Calf Wrap -
 AllCare Tubing
AllCare Tubing -
 AllCare Spikey Massage Ball
AllCare Spikey Massage Ball -
 AllCare Instant Cold Pack (15 x 25cm)
AllCare Instant Cold Pack (15 x 25cm) -
 AllCare Foam Roller Round
AllCare Foam Roller Round -
 Mueller Adjustable Calf / Shin Splint Support
Mueller Adjustable Calf / Shin Splint Support -
 Tubigrip
Tubigrip
To purchase physiotherapy products for a calf strain, click on one of the above links or visit the PhysioAdvisor Shop.
 More information
More information
- Initial Injury Management (R.I.C.E Regime)
- How to use Crutches.
- Ice or Heat.
- Achilles Tendon Taping.
- Calf taping.
- Why is my Injury not Improving?
- Calf Strain (Soleus)
- Lower Limb Injury Diagnosis Guide.
Become a PhysioAdvisor Member

Link to this Page
If you would like to link to this article on your website, simply copy the code below and add it to your page:
<a href="https://physioadvisor.com.au/injuries/lower-leg/calf-strain-gastrocnemius”>Calf Strain (Gastrocnemius) – PhysioAdvisor.com</a><br/>PhysioAdvisor offers detailed physiotherapy information on a calf strain including: symptoms, causes, diagnosis, treatment, exercises, physiotherapy products and more...
Return to the top of Calf Strain (Gastrocnemius).

