Patellar Tendonitis
Updated:
(Also known as Patellar Tendonitis, Patellar Tendinopathy, Patellar Tendinitis, Jumper’s Knee)
N.B. Although research suggests that ‘patellar tendinopathy’ is the more appropriate term to describe overuse injuries to the patellar tendon, we will use the term ‘patellar tendonitis’ in this document as it is more widely known.
What is patellar tendonitis?
Patellar tendonitis is a condition characterized by localised pain in the front of the knee (usually just below the knee cap) associated with tissue damage, disorganisation and sometimes swelling of the patellar tendon.
The large muscle at the front of your thigh is called the quadriceps (figure 1). This muscle attaches to the knee cap which in turn attaches to the tibia (shin bone) via the patellar tendon (figure 1).
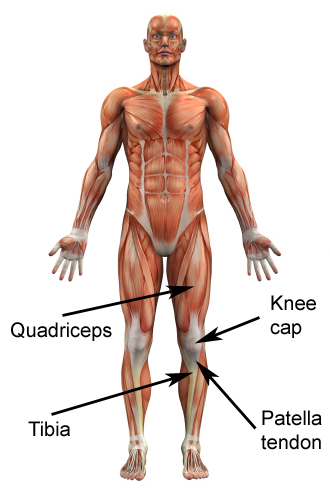
The quadriceps muscle is primarily responsible for straightening the knee (extension) and controlling bending of the knee (flexion) during weight bearing activity. It is particularly active during running, jumping, hopping, squatting, lunging and kicking. During contraction of the quadriceps, tension is placed on the patellar tendon via the patella. When this tension is excessive due to too much force and/or repetition, damage to the patellar tendon may occur. Patellar tendonitis is a condition whereby there is microscopic damage to the patellar tendon with subsequent degeneration, disorganisation and sometimes swelling of the tendon.
Patellar tendonitis most commonly affects young athletes (15 – 30 years of age), particularly men, who are involved in sports that repetitively load the patellar tendon. It is commonly seen in jumping sports, such as volleyball, basketball and netball.
Causes of patellar tendonitis
Patellar tendonitis most commonly occurs following a recent sudden change (or increase) in activity (i.e. “load” on the patellar tendon). This often involves starting a new unaccustomed activity or increasing the volume of an accustomed activity. Activities causing this condition usually entail repetitive or prolonged strain on the patellar tendon. Patellar tendonitis often occurs from repetitive running (particularly downhill), jumping, hopping or sudden deceleration activities (e.g. netball). It is particularly common in sports requiring frequent jumping and landing, such as basketball, volleyball, handball, football or netball.
Occasionally, patients may develop this condition suddenly due to a high force going through the patellar tendon beyond what it can withstand. This most commonly occurs when landing from a jump (particularly on hard surfaces) or during rapid acceleration whilst running. Occasionally the condition may occur due to direct trauma such as forceful blow to the patellar tendon.
Signs and symptoms of patellar tendonitis
Patients with this condition typically experience pain that develops gradually over time and is localised to the front of the knee just below the knee cap (i.e. the patellar tendon). In less severe cases, patients may only experience an ache or stiffness with rest (i.e. often at night or upon waking in the morning) following activities requiring forceful, repetitive or prolonged contraction of the quadriceps muscle. These activities typically include running (particularly up or down hills or stairs, or with rapid changes of direction), jumping, hopping, squatting or lunging.
The pain associated with this condition may also ‘warm up’ with activity in the initial stages of the injury. As the condition progresses, patients may experience symptoms that increase during activity and affect performance. Walking or standing may then be enough to aggravate symptoms.
Patients with this condition typically experience pain on firmly touching the patellar tendon (figure 1). An observable swelling or thickening of the tendon along with muscle wasting of the quadriceps may be evident (particularly in chronic cases) when compared to the unaffected side. Occasionally, a feeling of knee weakness may also be present particularly when attempting to jump or accelerate whilst running.
Diagnosis of patellar tendonitis
A thorough subjective and objective examination from a physiotherapist is usually sufficient to diagnose patellar tendonitis. Occasionally, an Ultrasound investigation may be required to assist with diagnosis and assess the severity of the condition. Further investigations, such as an X-ray or MRI may sometimes be indicated, usually to rule out other conditions.
Prognosis of patellar tendonitis
Most patients who suffer from patellar tendonitis heal well with appropriate physiotherapy and load management, and return to normal function in a number of weeks. Occasionally, rehabilitation can take significantly longer and may take many months in those who have had their condition for a long period of time. Early appropriate physiotherapy rehabilitation and treatment is vital to hasten recovery in all patients with this condition.
Treatment for patellar tendonitis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Contributing factors to the development of patellar tendonitis
There are numerous factors which can predispose patients to developing patellar tendonitis. These factors should be assessed and, where possible, corrected with direction from a physiotherapist. Some of these factors include:
- joint stiffness (particularly in the hip, knee or ankle)
- muscle tightness (particularly in the quadriceps, hip flexors, ITB, hamstrings or calf)
- muscle weakness (especially in the quadriceps, gluteals or calf)
- poor pelvic, hip or core stability
- inappropriate or excessive training
- inadequate recovery periods from training or activity
- change in training conditions,surfaces, footwear or technique
- inadequate warm up
- biomechanical abnormalities (e.g. flat or rigid feet)
- inappropriate footwear
- poor balance or control
- inadequate rehabilitation following a previous quadriceps or other lower limb injury
- being overweight
- diabetes
- genetic factors
Physiotherapy for patellar tendonitis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Other intervention for patellar tendonitis
Despite appropriate physiotherapy management, some patients with patellar tendonitis do not improve adequately. When this occurs the treating physiotherapist or doctor will advise on the best course of management. This may include further investigations such as X-rays, Ultrasound, MRI or CT scan, pharmaceutical intervention, corticosteroid injection, autologous blood injection, podiatrist or psychologist review or referral to appropriate medical authorities who will advise on any interventions that may be appropriate to improve the condition. In rare cases, where patients have been unresponsive to a high quality physiotherapy program and all other conservative measures, surgery may be indicated.
Exercises for patellar tendonitis
The following exercises are commonly prescribed to patients with patellar tendonitis. You should discuss the suitability of these exercises with your physiotherapist prior to beginning them. Generally, they should be performed 2 – 3 times daily and only provided they do not cause or increase symptoms.
Your physiotherapist can advise when it is appropriate to begin the initial exercises and eventually progress to the intermediate, advanced and other exercises. As a general rule, addition of exercises or progression to more advanced exercises should take place provided there is no increase in symptoms.
Initial Exercises
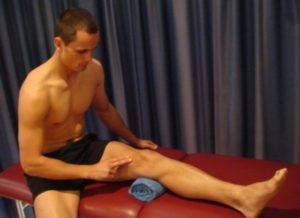
Static inner quadriceps contraction
Tighten the muscle at the front of your thigh (quadriceps) by pushing your knee down into a towel (figure 2). Put your fingers on your inner quadriceps (vastus medialis obliquus) to feel the muscle tighten during contraction. Hold for 5 seconds and repeat 4 times as hard as possible without increasing your symptoms. Once this is easy you can progress the exercise by holding the contraction for longer durations eventually building up to 45 second holds provided there is no increase in symptoms.
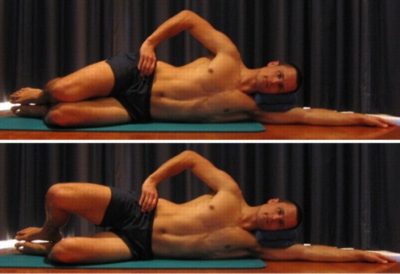
Clams
Begin this exercise lying on your side with your shoulders, hips and ankles in alignment. Your knees should be bent at right angles and resting together (figure 3). Slowly lift your upper knee away from your other leg, keeping your ankles together, your pelvis still and tightening your buttock muscles (gluteals). Hold for 2 seconds then slowly lower the knee back down. Repeat 10 – 20 times as far as possible provided the exercise is pain free.
Bridging
Begin this exercise lying on your back in the position demonstrated (figure 4). Slowly lift your bottom pushing through your feet, until your knees, hips and shoulders are in a straight line. Tighten your bottom muscles (gluteals) as you do this. Hold for 2 seconds then slowly lower your bottom back down. Repeat 10 – 30 times provided the exercise is pain free.


Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Intermediate Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Advanced Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Other Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Rehabilitation protocol for patellar tendonitis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
 Physiotherapy products for patellar tendonitis
Physiotherapy products for patellar tendonitis
Some of the most commonly recommended products by physiotherapists to hasten healing and speed recovery in patients with patellar tendonitis include:
To purchase physiotherapy products for patellar tendonitis, click on one of the above links or visit the PhysioAdvisor Shop.
 Find a Physio for patellar tendonitis
Find a Physio for patellar tendonitis
Find a physiotherapist in your local area who can assess and treat patellar tendonitis.
 More Exercises
More Exercises
- Quadriceps Strengthening Exercises.
- Quadriceps Flexibility Exercises.
- Knee Strengthening Exercises
- Knee Stretches
- Leg Strengthening Exercises
- Leg Stretches
- Lower Body Gym Exercises (Machine Weights)
- Lower Body Gym Exercises (Free Weights)
- Cardiovascular Exercise
- Balance Exercises
 More Information
More Information
- Patellar Tendon Taping
- How to use Crutches
- Ice or Heat
- R.I.C.E. Regime
- Do I Need Orthotics
- Choosing a Shoe
- Mechanical Pain
- Inflammatory Pain
- Understanding Pain
- Why is my injury not improving
- Return to Running
- Return to Sport
- Warming Up and Cooling Down
- Knee Diagnosis Guide
Become a PhysioAdvisor Member
-
 Individual Membership (12 Months)$59.95 for 1 year
Individual Membership (12 Months)$59.95 for 1 year -
 Individual Membership (3 Months)$39.95 for 3 months
Individual Membership (3 Months)$39.95 for 3 months -
 Individual Membership (Yearly)$49.95 / year
Individual Membership (Yearly)$49.95 / year -
 Individual Membership (Monthly)$15.95 / month
Individual Membership (Monthly)$15.95 / month

Link to this Page
If you would like to link to this article on your website, simply copy the code below and add it to your page:
<a href="https://physioadvisor.com.au/injuries/knee/patellar-tendonitis”>Patellar Tendonitis – PhysioAdvisor.com</a><br/>PhysioAdvisor offers detailed physiotherapy information on patellar tendonitis including diagnosis, treatment, exercises, products and more.
Return to the top of Patellar Tendonitis.