Hip Arthritis (Osteoarthritis)
Updated:
(Also known as Hip Osteoarthritis, Osteoarthritis of the Hip, Arthritis of the Hip, Degeneration of the Hip)
N.B. The term ‘hip arthritis’ will be used in this document to describe the condition known as hip osteoarthritis.
What is hip arthritis?
Hip arthritis is a condition characterized by a degenerative process whereby there is gradual wear and tear to the cartilage and bone surfaces of the hip joint with subsequent inflammation. This may occur following a specific injury or due to repetitive forces going through the hip beyond what it can withstand over a period of time.
In a normal hip, joint surfaces are smooth and there is cartilage between the bone ends which allow efficient shock absorption and smooth movement (figure 1).
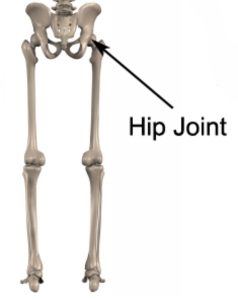
When the hip is damaged or overloaded, particularly with excessive weight-bearing or twisting forces, degeneration of the cartilage can occur reducing the hip’s shock absorbing capacity. As the condition progresses, and the cartilage wears away, the joint space can narrow and there is eventual wearing down of the bone ends so that the surfaces are no longer smooth. The bone ends may also develop small bony processes called ‘osteophytes’ (i.e. bone spurs). When some or all of these changes occur, the condition is known as hip arthritis.
Hip arthritis usually occurs after the age of 50 years. It is more common in those patients who are overweight or have a past history of injury, surgery or trauma to the hip.
Signs and symptoms of hip arthritis
Patients with this condition typically develop symptoms gradually over time. In individuals with minor cases of hip arthritis, little or no symptoms may be present. As the condition progresses, there may be increasing hip or groin pain with weight bearing activity and joint stiffness (particularly after rest or first thing in the morning). Severe joint pain, decreased hip flexibility, pain at night and grinding or clicking sensations during certain movements may also be experienced. The pain associated with hip arthritis is typically felt in the groin, front of the hip and/or the buttock region. Occasionally pain may be referred to the thigh or knee. Symptoms can sometimes fluctuate from month to month with patients reporting an increase in symptoms with colder weather. In more severe cases, muscle wasting (especially of the gluteals), and a limp may also be present.
Contributing factors to the development of hip arthritis
There are several factors which may contribute to the development of hip arthritis. These factors should be assessed and corrected (where possible) with direction from a physiotherapist and may include:
- age (> 40 years)
- being overweight
- genetics
- history of injury, surgery or trauma to the hip joint
- muscle weakness (particularly of the quadriceps and gluteals)
- muscle tightness (e.g. hip flexors, gluteals, adductors)
- stiffness in other joints (e.g. the thoracic or lumbar spine)
- a sedentary lifestyle
- leg length discrepancy or postural abnormalities of the lower limb
- poor biomechanics or foot posture (e.g. flat feet)
- inappropriate footwear
- poor core stability or balance
- excessive or inappropriate weight bearing or twisting activity
- inadequate recovery periods from training or activity
- poor nutrition or inappropriate diet
- hip joint bony abnormalities (which may result in hip impingement (femoroacetabular impingement) and subsequently increase the risk of developing arthritis).
Diagnosis of hip arthritis
A thorough subjective and objective examination from a physiotherapist may be sufficient to diagnose hip arthritis. An X-ray is usually required to confirm diagnosis. This may demonstrate signs of reduced joint space, irregularities of the bony ends and/or presence of bony spurs (osteophytes). Sometimes an MRI may also be indicated to assist with diagnosis and rule out other potential conditions.
It is important to note, however, that x-ray results do not necessarily always correlate well with the symptoms of the patient. A patient who is suffering severe pain due to hip arthritis can sometimes have x-rays which demonstrate only mild to moderate osteoarthritic changes. Conversely, a patient with only mild pain (or no symptoms) due to hip arthritis can sometimes have x-rays which demonstrate moderate to severe osteoarthritic changes. As such, both the patients’ symptoms, as well the investigation results are important in determining injury diagnosis and severity.
Treatment for hip arthritis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Prognosis for hip arthritis
Since hip arthritis is typically a progressive condition, complete resolution of symptoms is often not possible. However, in mild to moderate cases, most patients, if managed well, can maintain an active lifestyle with little or no symptoms and delay or prevent the deterioration of the condition. In severe cases that have been unresponsive to appropriate physiotherapy management and where quality of life is significantly affected, hip joint replacement surgery is often indicated with most patients subsequently experiencing a good outcome following the procedure.
Physiotherapy for hip arthritis
Physiotherapy treatment for patients with this condition is vital to delay hip joint deterioration, reduce symptoms, and improve strength, range of movement and function. Treatment may comprise:
- exercises to improve strength, flexibility, core stability, balance and function
- soft tissue massage
- electrotherapy (e.g. ultrasound)
- joint mobilization
- dry needling
- ice or heat treatment
- hydrotherapy
- education
- the use of crutches, a walking stick or other walking aids
- walking re-education
- activity and lifestyle modification advice
- biomechanical correction
- anti-inflammatory and supplement advice (e.g. fish oil, glucosamine and chondroitin)
- weight loss advice where appropriate
- advice on appropriate footwear or orthotics
Other intervention for hip arthritis
Despite appropriate physiotherapy management, some patients with arthritis of the hip continue to deteriorate. When this occurs, other intervention may be required. This may include pharmaceutical intervention, corticosteroid injection, the use of supplements such as fish oil, glucosamine and chondroitin, investigations such as an X-ray, CT scan, bone scan or MRI, or assessment from a specialist.
In more advanced cases of hip arthritis, where symptoms are severe, patients may require surgical intervention. This may involve a hip arthroscope or hip joint replacement surgery. The treating physiotherapist or doctor can advise if this may be required and will refer to an orthopaedic specialist for an assessment and opinion. Occasionally referral to a podiatrist (for orthotics) or to a nutritionist (to assist with body weight reduction) may be appropriate.
Hip joint replacement surgery for hip arthritis
Hip joint replacement surgery for patients with this condition is usually considered where pain is unrelenting, there is significantly reduced function and conservative measures have failed to improve symptoms. Following a total hip joint replacement, patients are normally in hospital for 5 to 10 days and require physiotherapy treatment and rehabilitation from day 1 onwards. Resumption of normal daily activity can usually be achieved 3 – 6 months following surgery.
Exercises for hip arthritis
The following exercises are commonly prescribed to patients with this condition. You should discuss the suitability of these exercises with your physiotherapist prior to beginning them. Generally, they should be performed 3 times daily and only provided they do not cause or increase symptoms.
Your physiotherapist can advise when it is appropriate to begin the initial exercises and eventually progress to the intermediate, advanced and other exercises. As a general rule, addition of exercises or progression to more advanced exercises should take place provided there is no increase in symptoms.
Initial Exercises
Hip Flexion
Begin this exercise lying on your back (figure 2). Slowly take your knee to your chest as far as you can go without pain and provided you feel no more than a mild to moderate stretch, then lower back down. Repeat 10 – 20 times provided there is no increase in symptoms.
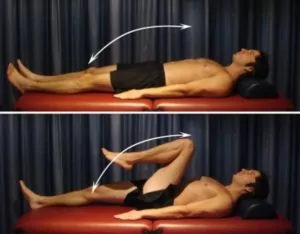
Hip Abduction
Begin this exercise lying on your back (figure 3). Keeping your knee straight, take your leg to the side as far as you can go without pain and provided you feel no more than a mild to moderate stretch, then return to the starting position. Keep your knee cap and toes facing the ceiling throughout the exercise. Repeat 10 – 20 times provided there is no increase in symptoms.

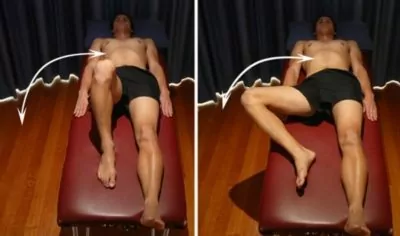
Hip External Rotation
Begin this exercise lying on your back with your knee bent and foot flat on the floor (figure 4). Take your knee to the side as far as you can go without pain and provided you feel no more than a mild to moderate stretch, then return to the starting position. Repeat 10 – 20 times provided there is no increase in symptoms.
Intermediate Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Advanced Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Other Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Rehabilitation Protocol for hip arthritis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
 Physiotherapy products for hip arthritis
Physiotherapy products for hip arthritis
Some of the most commonly recommended products by physiotherapists to hasten healing and speed recovery in patients with this condition include:
To purchase physiotherapy products for hip arthritis click on one of the above links or visit the PhysioAdvisor Shop.
 Find a Physio for hip arthritis
Find a Physio for hip arthritis
Find a physiotherapist in your local area who can treat this condition.
 More Exercises for hip arthritis
More Exercises for hip arthritis
- Hip Flexibility Exercises
- Hip Strengthening Exercises
- Balance Exercises
- Cardiovascular Exercise
- Beginner Pilates Exercises
- Leg Strengthening Exercises
- Leg Stretches
- Machine Weights (Lower Body)
 Recommended Reading
Recommended Reading
- Ice or Heat
- The R.I.C.E. regime
- Choosing a Shoe
- Do I Need Orthotics?
- How to use Crutches
- Understanding Pain
- Hip Diagnosis Guide
Become a PhysioAdvisor Member
-
 Individual Membership (12 Months)$59.95 for 1 year
Individual Membership (12 Months)$59.95 for 1 year -
 Individual Membership (3 Months)$39.95 for 3 months
Individual Membership (3 Months)$39.95 for 3 months -
 Individual Membership (Yearly)$49.95 / year
Individual Membership (Yearly)$49.95 / year -
 Individual Membership (Monthly)$15.95 / month
Individual Membership (Monthly)$15.95 / month

Link to this Page
If you would like to link to this article on your website, simply copy the code below and add it to your page:
<a href="https://physioadvisor.com.au/injuries/hip-groin/hip-arthritis-osteoarthritis”>Hip Arthritis (Osteoarthritis) – PhysioAdvisor.com</a><br/>PhysioAdvisor offers detailed physiotherapy information on hip arthritis (hip osteoarthritis) including diagnosis, treatment, exercises and more.
Return to the top of Hip Arthritis (Osteoarthritis).









