Shoulder Arthritis (Osteoarthritis)
Updated:
(Also known as Shoulder Arthritis, Shoulder Osteoarthritis, Shoulder Degeneration, Arthritis of the Shoulder)
N.B. There are numerous types of shoulder arthritis (e.g. shoulder rheumatoid arthritis, shoulder osteoarthritis etc.). The term ‘shoulder arthritis’ will be used in this document to describe the condition known as shoulder osteoarthritis.
What is shoulder arthritis?
Shoulder arthritis is a condition characterized by gradual wear and tear to the ball and socket joint of the shoulder. This results in inflammation and degeneration to the cartilage and bone surfaces of the shoulder joint with subsequent pain and stiffness.
The shoulder joint is a ball and socket joint. The ball originating from the upper aspect of the humerus (upper arm bone). The shoulder blade (scapula) giving rise to the socket (figure 1).
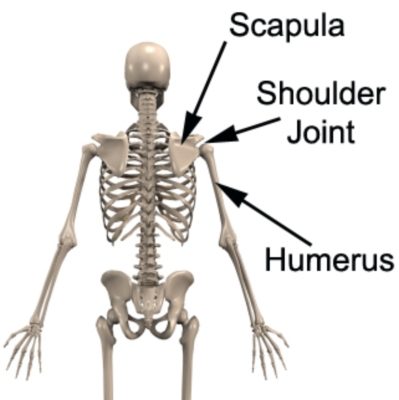
In a normal shoulder, joint surfaces are smooth, congruent and lined with shock absorbing cartilage. This allows efficient movement and normal shoulder function.
When the shoulder joint is injured (due to repetitive, prolonged or sometimes traumatic forces), damage and degeneration of the shock absorbing cartilage may occur. This impairs the joint’s ability to withstand stress therefore placing additional load on the cartilage and bone surfaces of the shoulder during activity. As the cartilage continues to wear away, the joint space of the shoulder can narrow and there is eventual wearing down of the bone ends so that surfaces are no longer smooth. With further progression of the condition, thickening of the joint capsule and bony spurs (known as osteophytes) may begin to develop in response to the increased stress on the joint. When some or all of these degenerative changes take place, the condition is known as shoulder arthritis.
Shoulder arthritis is relatively common in clinical practice and typically affects an older population (> 50 years of age).
What is the cause of shoulder arthritis?
Shoulder arthritis typically occurs due to repetitive or prolonged stress on the shoulder joint beyond what it can withstand over a period of time. This causes gradual wear and tear to the joint surfaces of the shoulder. Structures affected may include the articular cartilage, labrum (a continuation of the cartilage), joint capsule and bone surfaces. Provocative activities often involve repetitive, prolonged or forceful use of the shoulder such as lifting, carrying, overhead activity, pushing or pulling, use of the arms in front of the body or weight bearing activity (including lying on the affected shoulder).
Shoulder arthritis may also occur following shoulder surgery or traumatic injuries to the shoulder. Surgery or trauma may change or damage the joint surfaces or alter shoulder mechanics predisposing the joint to further degeneration. Injuries associated with shoulder arthritis may include shoulder dislocation, subluxation, fracture, labral tear, rotator cuff injury or avascular necrosis (death of bone due to blood vessel interruption).
Patients may also develop the condition in association with a shoulder joint infection or rheumatological condition. Excessive alcohol consumption, use of certain medication (such as corticosteroids) or exposure to radiation may also increase the likelihood of the condition occurring.
What are the signs and symptoms of shoulder arthritis?
Shoulder arthritis is a condition that typically develops gradually over a period of time. In patients with minor shoulder arthritis, little or no symptoms may be experienced. As the condition develops and further degeneration takes place, increasing joint pain and stiffness may be present (particularly with rest or upon waking first thing in the morning).
Other associated symptoms vary based on the severity of the condition and may include:
- shoulder pain that may radiate into the upper arm
- tenderness on firmly touching the affected joint
- observable joint enlargement and swelling
- reduced shoulder flexibility and strength
- functional limitation
- audible or palpable clicking or grinding sensations during movement
- locking of the shoulder (where it gets stuck and you have to work it out)
- catching pain
- severe joint pain
- night or morning pain (that often eases with movement or a hot shower)
- difficulty sleeping (particularly on the affected side)
- muscle wasting of the shoulder
- Increasing symptoms with colder weather
How is shoulder arthritis diagnosed?
A thorough examination from a physiotherapist may be sufficient to diagnose shoulder arthritis. Observable radiological changes to the shoulder joint (typically in the form of an X-Ray) are usually required to confirm diagnosis and assess the severity of the condition. X-Rays may demonstrate reduced joint space, bony irregularity and the presence of osteophytes (bony spurs). MRI or CT scan investigation may sometimes be indicated to assist diagnosis and rule out the presence of other conditions.
What is the treatment for shoulder arthritis?

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Surgery for shoulder arthritis
For those patients with severe shoulder arthritis that is unresponsive to conservative management and who have ongoing significant pain and disability, surgical intervention may be indicated to provide the best outcome. Surgery for shoulder arthritis usually involves partial or complete joint replacement (arthroplasty) with lengthy rehabilitation to follow. Shoulder replacements also have a limited lifespan and may not be appropriate for younger patients. Occasionally shoulder arthroscopy (‘key hole surgery’) may be indicated to remove loose pieces of damaged cartilage. The treating physiotherapist and doctor will refer to a specialist if surgery may be indicated. Physiotherapy treatment and rehabilitation is then required following surgery, to ensure an optimal outcome and enable a safe return to activity.
What is the prognosis of shoulder arthritis?
Since little can be done to reverse the degenerative changes associated with this condition, complete resolution of symptoms may not be possible. However, most patients with mild to moderate shoulder arthritis who are managed appropriately can maintain an active lifestyle with little or no symptoms and delay or prevent the deterioration of the condition. In severe cases that have been unresponsive to high quality physiotherapy management and where significant pain and disability is present, joint replacement surgery may be indicated with lengthy rehabilitation to follow.
Contributing factors to the development of shoulder arthritis
There are several factors which can predispose patients to developing shoulder arthritis. These need to be assessed and corrected where possible with direction from a physiotherapist. Some of these factors include:
- prior shoulder trauma (such as dislocation, fracture, subluxation or avascular necrosis)
- inadequate rehabilitation following a previous shoulder injury
- excessive or inappropriate training or activity using the shoulder
- inadequate rest periods from training or activity
- abnormal biomechanics
- poor posture
- muscle tightness or imbalances
- neck, upper back and shoulder stiffness
- muscle weakness (especially the scapular stabilizers and rotator cuff muscles)
- inadequate warm-up
- poor nutrition or inappropriate diet
- excessive alcohol consumption
- obesity
- excessive corticosteroid therapy
- exposure to radiation
- presence of rheumatological conditions or osteoporosis
- prior shoulder surgery
- age > 50 years
Physiotherapy treatment for shoulder arthritis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Other intervention for shoulder arthritis
Despite appropriate physiotherapy rehabilitation and management, some patients with this condition continue to deteriorate or fail to improve sufficiently either conservatively or following surgery. When this occurs the treating physiotherapist or doctor can advise on the best course of management. This may include further investigations such as X-rays, Ultrasound, MRI or CT scans, prescription of medication, corticosteroid injection, the use of natural supplements (such as fish oil), chronic pain management or further surgery (such as shoulder arthroscopy, or a partial or complete joint replacement).
Exercises for shoulder arthritis
The following exercises are commonly prescribed to patients with shoulder arthritis. You should discuss the suitability of these exercises with your physiotherapist prior to beginning them. Generally, they should be performed 2 – 3 times daily and only provided they do not cause or increase symptoms.
Your physiotherapist can advise when it is appropriate to begin the initial exercises and eventually progress to the intermediate, advanced and other exercises. As a general rule, addition of exercises or progression to more advanced exercises should take place provided there is no increase in symptoms.
Initial Exercises for shoulder arthritis
Shoulder Blade Squeezes
Begin sitting or standing tall with your back straight (figure 2). Your chin should be tucked in slightly and your shoulder blades should be back slightly. Slowly squeeze your shoulder blades together as hard and far as possible provided it does not cause or increase symptoms. Hold for 5 seconds and repeat 10 times provided the exercise is pain free.
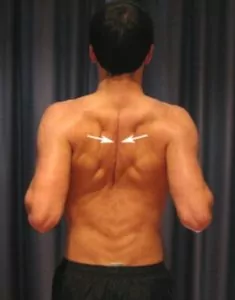
Pendular Exercises
Begin this exercise by leaning forwards with the forearm of your uninjured arm supported on a table or bench (figure 3). Keeping your back straight and your shoulder relaxed, gently swing your affected arm forwards and backwards as far as you can go without pain and provided you feel either nothing, or, no more than a mild to moderate stretch. Repeat 10 times provided the exercise does not cause or increase symptoms. Repeat the exercise swinging your arm side to side provided it is pain free.
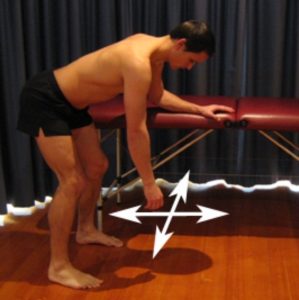
Pendular Circles
Begin this exercise by leaning forwards with the forearm of your uninjured arm supported on a table or bench (figure 4). Keeping your back straight and your shoulder relaxed, gently swing your affected arm in circles clockwise as far as you can go without pain and provided you feel either nothing, or, no more than a mild to moderate stretch. Repeat the exercise swinging your arm counter clockwise. Repeat 10 times in each direction provided there is no increase in symptoms.
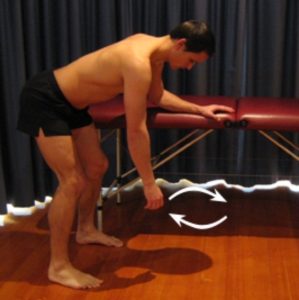
More Initial Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Intermediate Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Advanced Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Other Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Rehabilitation protocol for shoulder arthritis

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
 Physiotherapy products for shoulder arthritis
Physiotherapy products for shoulder arthritis
Some of the most commonly recommended products by physiotherapists to hasten healing and speed recovery in patients with shoulder arthritis include:
To purchase physiotherapy products for an arthritic shoulder click on one of the above links or visit the PhysioAdvisor Shop.
 Other Exercises for shoulder arthritis
Other Exercises for shoulder arthritis
- Shoulder Stretches
- Shoulder Strengthening Exercises
- Scapula Stability Exercises.
- Rotator Cuff Strengthening Exercises.
- Upper Body Massage Ball Exercises.
- Neck Stretches
- Postural Exercises
- Arm Strengthening Exercises.
- Upper Body Machine Weights.
- Cable Exercises (Back & Biceps)
- Cable Exercises (Chest, Shoulders & Triceps).
- Free Weights (Back & Biceps).
- Free Weights (Chest, Shoulders & Triceps).
 Useful Links for Shoulder Arthritis
Useful Links for Shoulder Arthritis
- Shoulder Taping
- Postural Taping.
- Posture.
- Ice or Heat.
- The R.I.C.E. Regime.
- Injury Prevention.
- Investigations.
- Inflammatory Pain.
- Mechanical Pain.
- Understanding Pain.
- Returning to Sport.
- Warming up and Cooling Down.
- Why is My Injury not Improving?
- Shoulder Diagnosis Guide.
 Find a Physio for shoulder arthritis
Find a Physio for shoulder arthritis
Find a physiotherapist in your local area who can treat shoulder osteoarthritis.
Become a PhysioAdvisor Member
-
 Individual Membership (12 Months)$59.95 for 1 year
Individual Membership (12 Months)$59.95 for 1 year -
 Individual Membership (3 Months)$39.95 for 3 months
Individual Membership (3 Months)$39.95 for 3 months -
 Individual Membership (Yearly)$49.95 / year
Individual Membership (Yearly)$49.95 / year -
 Individual Membership (Monthly)$15.95 / month
Individual Membership (Monthly)$15.95 / month

Link to this Page
If you would like to link to this article on your website, simply copy the code below and add it to your page:
<a href="https://physioadvisor.com.au/injuries/shoulder/shoulder-arthritis-osteoarthritis”>Shoulder Arthritis (Osteoarthritis) – PhysioAdvisor.com</a><br/>Comprehensive information on shoulder arthritis by experienced physiotherapists. Including symptoms, causes, treatment, exercises, rehab protocol and more.
Return to the top of Shoulder Arthritis (Osteoarthritis).









